Imagine visiting eight doctors before finally getting the right diagnosis for the serious, debilitating condition that has been complicating your life for years. This challenging ordeal is a reality for many people suffering from a mitochondrial disease, who often require a team of specialists to help identify and care for their specific needs.1
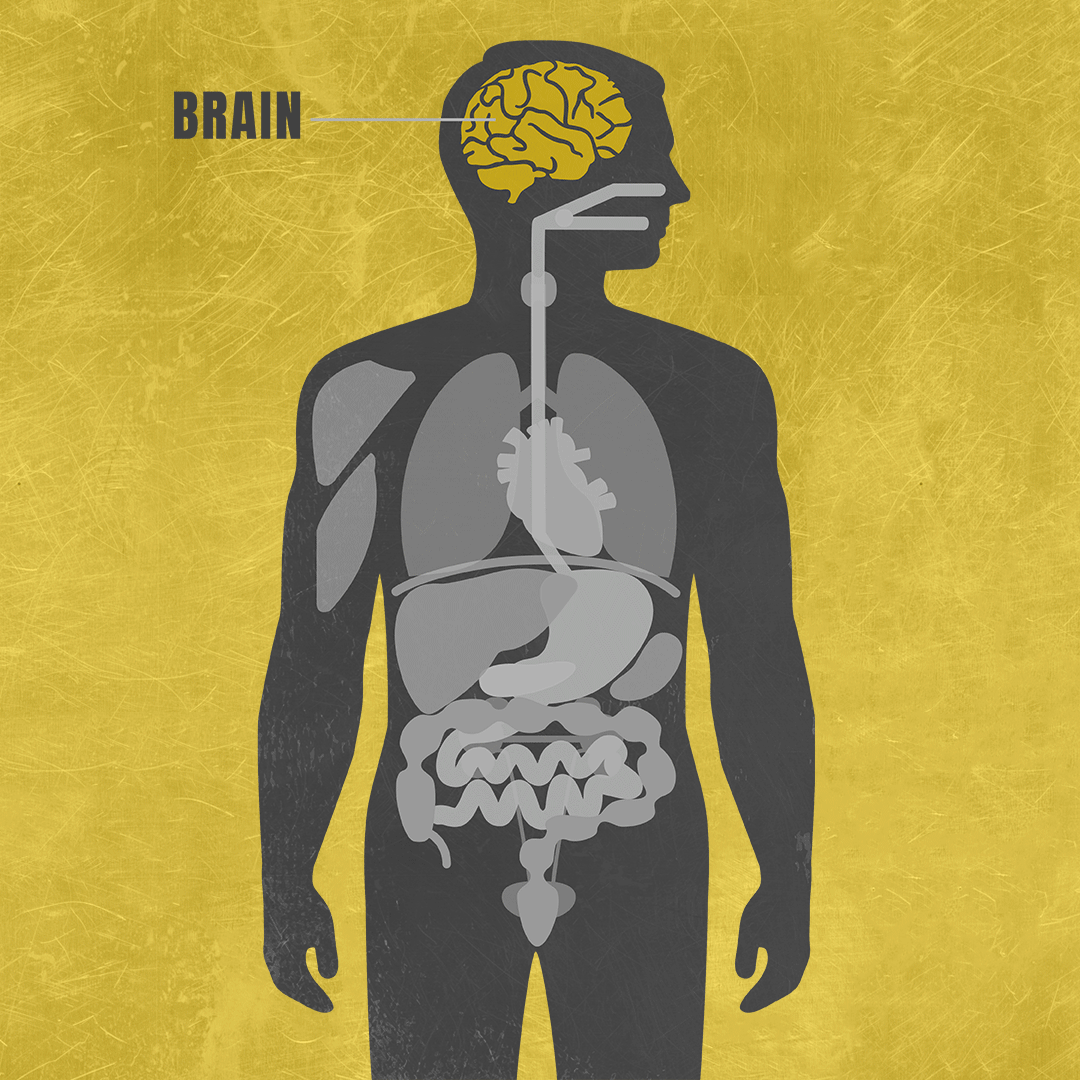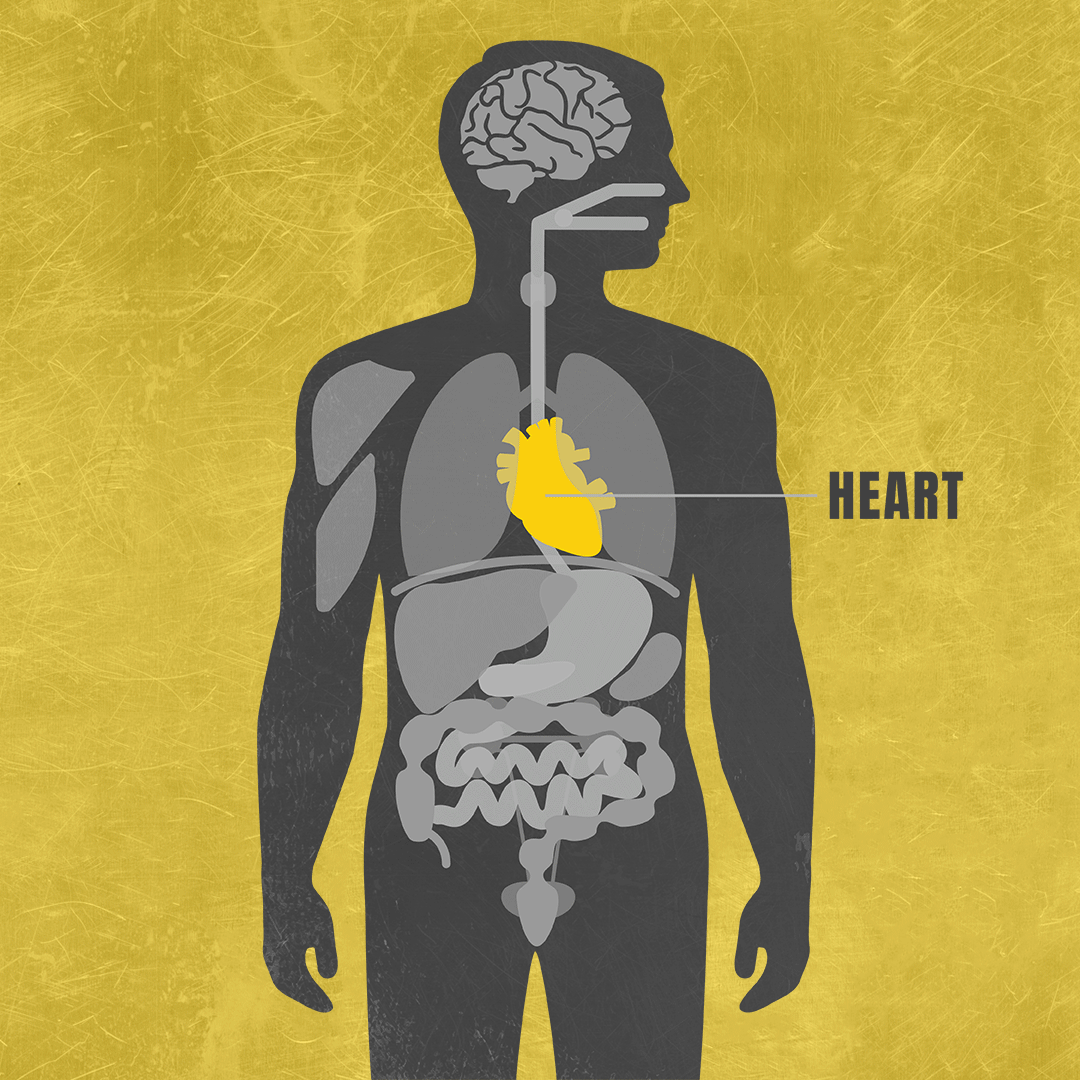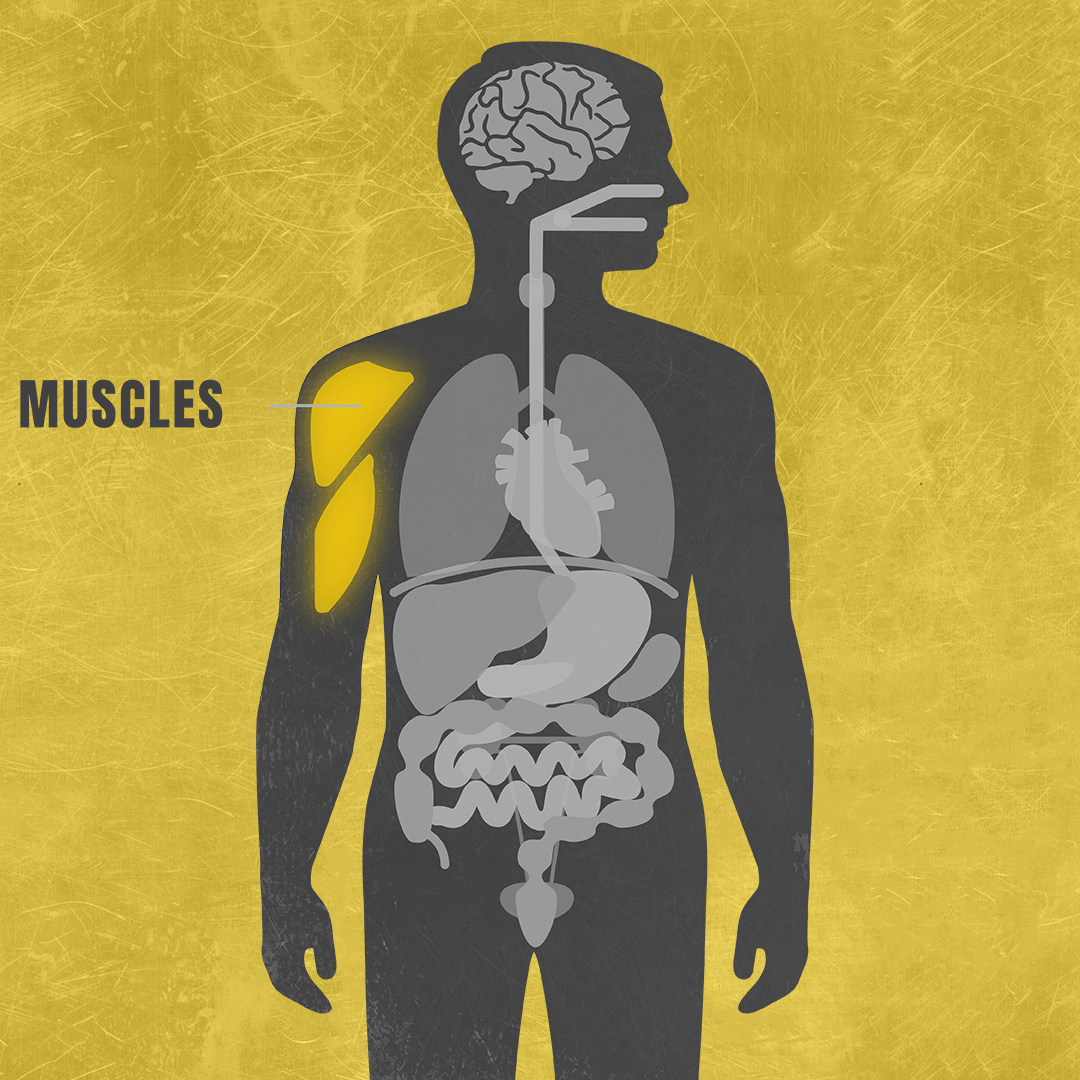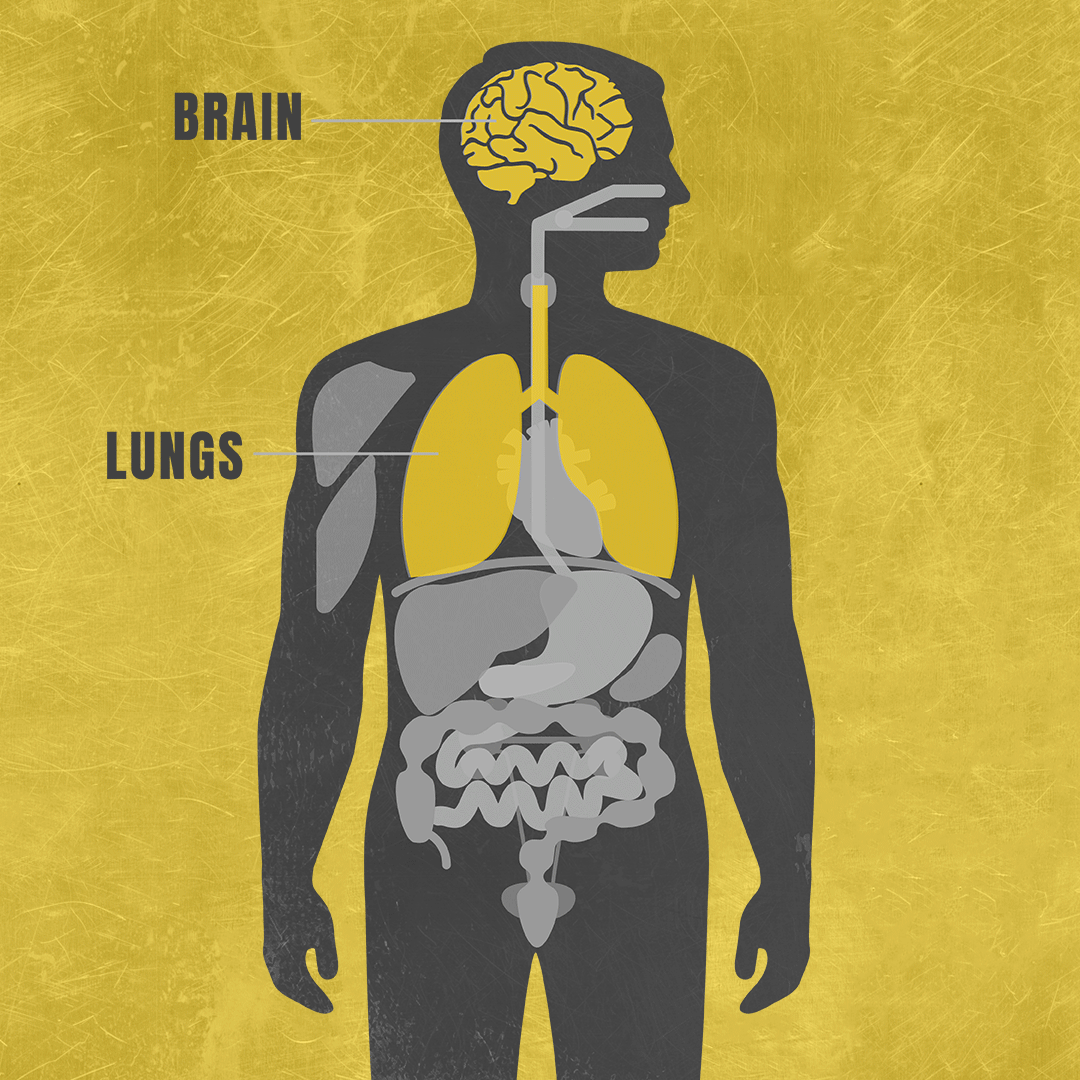
Mitochondrial diseases are difficult to diagnose in part because they have a wide range of effects on the body, often varying from one person to another.2,3 Because mitochondrial diseases limit how much energy the cells in your body produce, they typically affect at least three different organ systems, such as the brain, lungs and muscles.4
Comorbidities in Mitochondrial Diseases5
Multiple conditions occurring at the same time are known as comorbidities. Common comorbidities in people with mitochondrial diseases include seizures, asthma, heart failure and diabetes, among others. Comorbidities affect the cost and burden of mitochondrial diseases, for both patients and caregivers, due to the multisystem nature of the disease and the need for a coordinated care team across medical specialties.
Below you’ll learn about some of the most common comorbidities in children and adults with mitochondrial diseases.
Comorbidities in Children with Mitochondrial Diseases5
Children with mitochondrial diseases are most frequently affected by neurological disorders, respiratory diseases, immune disorders and cardiac conditions.
- Neurological and neuromuscular disorders
- Neurological disorders are the most common comorbidities in children with mitochondrial diseases.
- Children with mitochondrial diseases are affected by seizure disorders (nearly 50%) and autistic disorders (nearly 25%).
- Other conditions include spina bifida, cerebral palsy, Parkinson’s disease and Huntington’s disease.
- Respiratory disorders
- Nearly a third of children with mitochondrial diseases suffer from asthma.
- Other respiratory disorders include respiratory distress syndromes and cardio-respiratory failure and shock.
- Cardiac disorders
- Congestive heart failure affects 12% of children with mitochondrial disease, likely due to the high-energy requirements of the heart muscles.
- Other cardiac disorders include heart defects and circulatory disorders.
- Immune system disorders
- Common immune system disorders in children with mitochondrial diseases include myasthenia gravis and Guillain Barre syndrome.
Comorbidities in Adults with Mitochondrial Diseases5
In adults with mitochondrial diseases, common comorbidities fall into the following categories: diabetes, respiratory disorders, neurological disorders and cardiac disorders.
- Diabetes
- Diabetes is the most common comorbidity in adults with mitochondrial diseases, occurring in one third of patients.
- Respiratory disorders
- Asthma is the most common comorbid respiratory disorder in adults with mitochondrial diseases, occurring in nearly a quarter of patients.
- Other common respiratory disorders include cardio-respiratory failure and shock, respiratory distress syndromes and chronic obstructive pulmonary disease.
- Neurological disorders
- The most common neurological disorders in adults with mitochondrial diseases are seizures and convulsions (23% of patients).
- Other neurological disorders include major depressive disorder and bipolar disorder.
- Cardiac disorders
- Congestive heart failure is the most common cardiac condition (17% of patients), followed by heart arrhythmias (13.6%).
Coordinating Your Care Team
A coordinated care team of doctors and specialists can help treat the various individual components of mitochondrial diseases. A patient’s team may include neurologists, gastroenterologists, cardiologists, ophthalmologists, pediatricians and physical therapists among other specialists, depending on individual needs. Speak with your physicians to determine what is right for you.
There is a need for greater education about mitochondrial diseases in routine clinical care since the disease is often mistaken for other, more common conditions. Educating yourself and becoming an advocate for yourself or your loved one are important when dealing with conditions as complicated as mitochondrial diseases. Learn more about the symptoms and diagnosis of mitochondrial disease.
####
Ref. 1 Pfeffer G and Chinnery PF. Diagnosis and treatment of mitochondrial myopathies. Ann Med. 2013 Feb;45(1):4-16.
Ref. 2 The Charge. Recognizing key symptoms of mitochondrial disease. Available at: https://www.thecharge.com/recognizing-key-symptoms-of-mitochondrial-disease/ Accessed September 2019.
Ref. 3 Alston CL, Rocha MC, Lax NZ, et. al. The genetics and pathology of mitochondrial disease. J Pathol. 2017 Jan; 241(2):236-250.
Ref. 4 The Charge. Diagnosing mitochondrial disease. Available at: https://www.thecharge.com/diagnosing-mitochondrial-disease/ Accessed September 2019.
Ref. 5 Cohen B, Balcells C, Hotchkiss B, et al. A retrospective analysis of health care utilization for patients with mitochondrial disease in the United States: 2008-2015. Orphanet Journal of Rare Diseases. 2018;13:210.